New Kaiser Permanente study highlights importance of monitoring for signs of heart failure after hospital discharge
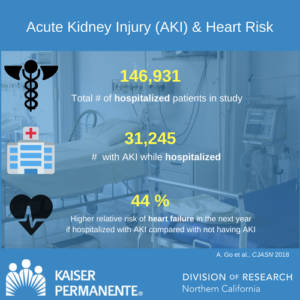 OAKLAND, Calif., May 16, 2018 — Hospitalized patients who experience acute kidney injury face a 44 percent greater risk of heart failure during their first year after leaving the hospital, according to new Kaiser Permanente research published today in the Clinical Journal of the American Society of Nephrology (CJASN).
OAKLAND, Calif., May 16, 2018 — Hospitalized patients who experience acute kidney injury face a 44 percent greater risk of heart failure during their first year after leaving the hospital, according to new Kaiser Permanente research published today in the Clinical Journal of the American Society of Nephrology (CJASN).
Acute kidney injury is a sudden decline in the ability of the kidneys to perform their normal function of filtering waste products from blood. People who are hospitalized for a wide variety of conditions, from major surgery to severe infection, are at risk for acute kidney injury, which can increase a patient’s long-term risk of death even after they are successfully treated and sent home.
“While Kaiser Permanente has had success in lowering rates of acute kidney injury in hospitalized patients, rates are rising nationwide, and even minor injury is linked to a higher risk of death,” said Alan S. Go, MD, director of the Comprehensive Clinical Research Unit within the Kaiser Permanente Northern California Division of Research and lead author of the new study.
Earlier research by Dr. Go and colleagues linked hospitalized acute kidney injury to elevated risk of high blood pressure, but how it increases overall risk of death is still unclear. “Cardiovascular disease could be part of the equation,” Go said.

In the new study, the research team examined electronic health records of patients who were admitted to one of Kaiser Permanente Northern California’s 21 hospitals at some point between 2006 and 2013. They investigated whether the risk of various cardiovascular events within one year of leaving the hospital differed between patients who experienced acute kidney injury while hospitalized and those who did not.
Out of 146,931 hospitalized patients included in the analysis, 31,245 experienced acute kidney injury. To help ensure an accurate comparison, patients with acute kidney injury were statistically matched to patients without acute kidney injury according to similar demographics, length of hospital stay, medications they took, how acutely ill they were, and other characteristics.
About 1 in 25 people who are hospitalized for any reason will experience heart failure within a year. The analysis found that even after accounting for remaining differences, patients with hospitalized acute kidney injury experienced a 44% higher relative risk of heart failure within one year of hospital discharge, compared to those without acute kidney injury. Rates of other cardiovascular events linked to atherosclerosis (narrowing of the arteries) did not differ significantly between the two groups.
“The number of atherosclerotic events in patients with acute kidney injury was lower than we expected,” Dr. Go said. “Overall, our results highlight heart failure as a key risk for patients who experienced acute kidney injury in the hospital.”
According to senior author Kathleen D. Liu, MD, PhD, of the University of California, San Francisco, the new findings suggest the need for doctors to be more vigilant in looking for signs of heart failure in patients who experienced hospitalized acute kidney injury. “Earlier detection of heart failure symptoms in these patients could potentially save lives.”
Meanwhile, Dr. Go and others are working to tease out the mechanisms underlying the increased risk. “Kidney damage affects a number of biological pathways, including inflammation and mineral metabolism,” Dr. Go said. “If we could understand how these changes increase risk of heart failure, we may be able to develop new strategies for prevention.”
Additional co-authors on the study were Chi-yuan Hsu, MD, MSc, Jingrong Yang, MA, and Thida C. Tan, MPH, of the Kaiser Permanente Division of Research; and Sijie Zheng, MD, PhD, and Juan D. Ordonez, MD, MPH, of the Kaiser Permanente Oakland Medical Center.
This research was funded by the National Institute of Diabetes and Digestive and Kidney Diseases.




This Post Has 0 Comments