In large Kaiser Permanente study, visceral and intramuscular fatness increased cardiovascular risk, even among normal-weight women.

Body composition, especially excess central adiposity or intra-abdominal fat, can result in an increased risk of cardiovascular disease in normal-weight breast cancer survivors, a large new Kaiser Permanente study shows.
“Cardiovascular disease is a major source of morbidity and mortality among breast cancer survivors,” said lead author Elizabeth Cespedes Feliciano, ScD, research scientist in the Kaiser Permanente Northern California Division of Research. “Normal-weight people aren’t generally considered at risk for cardiovascular disease. But many of them have an abnormal adipose tissue distribution, and we need to pay attention to them.”
The study, “Adipose Tissue Distribution and Cardiovascular Disease Risk among Breast Cancer Survivors,” was published today in the Journal of Clinical Oncology.
Most cardiovascular research among cancer survivors has relied on body mass index (BMI) as a measure of adiposity, or excess fat in the body, Feliciano said. “This study is unique in that we were able to review nearly 3,000 computed tomography (CT) scans taken of breast cancer patients. While these scans were taken for patient diagnosis and surveillance, we used them to accurately measure where adipose tissue was stored in the body.”
Where fat is stored matters to cardiovascular health
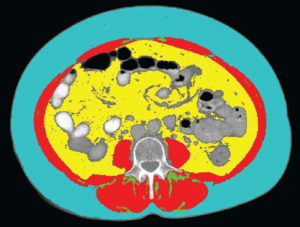
The body can store fat in different locations. In this study, the researchers examined body fatness or adiposity stored in these locations:
- * Subcutaneous: fat stored in adipose tissue cells underneath the skin but outside the abdominal muscle wall.
- * Visceral: fat stored in adipose tissue cells around organs inside the abdomen.
- * Intramuscular: fat droplets stored within muscle tissue cells.
“When fat collects in muscles and around the organs it promotes inflammation and insulin resistance, which can in turn contribute to cardiovascular disease,” Feliciano said.
Greater visceral and intramuscular adiposity increased cardiovascular risk by 15% and 21%, respectively, in all of the women studied. In normal-weight women, greater visceral adiposity increased cardiovascular risk by 70%, independent of cancer treatments and pre-existing cardiovascular risk factors such as diabetes, high blood pressure, and dyslipidemia (an abnormal level of lipids, or fats, in the blood).
When the researchers examined BMI categories, which are more-often used clinically, only severely obese women had an increased cardiovascular risk; there was no increased risk in the lower BMI categories.
“The greatly increased cardiovascular risk among normal-weight patients with visceral adiposity would go undetected with BMI alone,” said senior author Bette J. Caan, DrPH, senior research scientist at the Division of Research.
Body composition vs. BMI

Caan co-authored recent research published in JAMA Oncology, which identified a similar increase in heart risks in colorectal cancer patients who had greater visceral and intramuscular adiposity, as well as a study in JAMA Network Open, which found an increased risk of both cardiovascular and cancer mortality in normal-weight women who had central obesity.
Feliciano said that clinicians, including the cancer care team, should consider body composition in addition to BMI when assessing the risk of heart disease in breast cancer patients. “Waist circumference can serve as a simple proxy for central obesity, and CT scans — which are often available in cancer patients — can also be used to help to identify patients with excess adiposity at risk of cardiovascular disease,” she said.
Caan is principal investigator of the ongoing FORCE trial, which is testing a resistance-training intervention in cancer patients to help optimize body composition during cancer treatment.
“We know that resistance training is safe during active chemotherapy. It’s effective in building muscle and reducing intramuscular and visceral adiposity, and it has known benefits for improving short-term measures of cardiovascular risk,” Feliciano said. “Resistance training has a lot of potential for benefit and little potential for harm in cancer patients.”
The National Cancer Institute (R01CA184953) supported this study, and Feliciano was additionally supported by K01CA226155.
In addition to Feliciano and Caan, co-authors were Wendy Y. Chen, MD, MPH, Dana Farber Cancer Institute; Patrick T. Bradshaw, PhD, University of California, Berkeley; Carla M. Prado, PhD, University of Alberta, Edmonton; and Stacey Alexeeff, PhD, Kathleen B. Albers, MPH, and Adrienne L. Castillo, MS, Kaiser Permanente Northern California Division of Research.





This Post Has 0 Comments