David Vinson, MD, has been conducting research on nights and weekends for much of his 17-year career as an emergency-room physician in The Permanente Medical Group. Now a new program sponsored by TPMG will allow him to dedicate a portion of his clinical work week to research, while collaborating with investigators at the Division of Research (DOR).
“The Physician Researcher Program offers an opportunity for a group of physicians to devote part of their careers to conducting research,” says Philip Madvig, MD, TPMG associate executive director. “We will invest in them becoming researchers, while they remain active in clinical practice the majority of the time.”
Starting in July of this year, the six physicians in the inaugural class of the Physician Researcher Program will devote 20 to 40 percent of their time to research projects that are designed to systematically evaluate clinical care. Then the physician researchers will have the opportunity to disseminate and implement the relevant learnings across Kaiser Permanente Northern California.
Meet the Division of Research’s inaugural class of physician researchers
“This is such a wonderful opportunity to work alongside bright, energetic researchers, who are all eager to translate their creative research ideas into studies that will improve patient care,” says Dr. Vinson, who practices at Kaiser Permanente’s Roseville and Sacramento Medical Centers.
Learning health care system
TPMG has supported clinical and health systems research since the 1940s, when Morris Collen, MD, published studies reporting on use of the “wonder drug” penicillin in workers at the Kaiser shipyards in Richmond. The TPMG Department of Medical Methods Research, which was founded by Dr. Collen in 1961 and is now known as the Division of Research, currently supports hundreds of studies conducted by more than 50 investigators and several hundred clinicians, primarily with federal and institutional funding.
The DOR helps TPMG physicians with consultations and research project support via its Comprehensive Clinical Research Unit and its Biostatistical Consulting Unit. It manages Kaiser Permanente’s Community Benefit research grants program, which supports short-term projects. In recent years, the Division’s Delivery Science Research Program and Rapid Analytics Unit, supported by TPMG, have been partnering researchers with clinicians to answer clinical questions that can be quickly translated into care-delivery improvements.
The Physician Researcher Program expands on this delivery science portfolio by designating a team of TPMG clinicians to conduct research that transforms how care is delivered, while they also continue to make their clinical contributions.
“I don’t believe there’s a health care system or academic medical center in the country that has formed a program like this—it’s unique,” says Tracy A. Lieu, MD, MPH, director of the Division of Research. “It’s a way of positioning TPMG at the national forefront of what we think will be a wave of activity among health care systems that want to call themselves learning health care systems.”
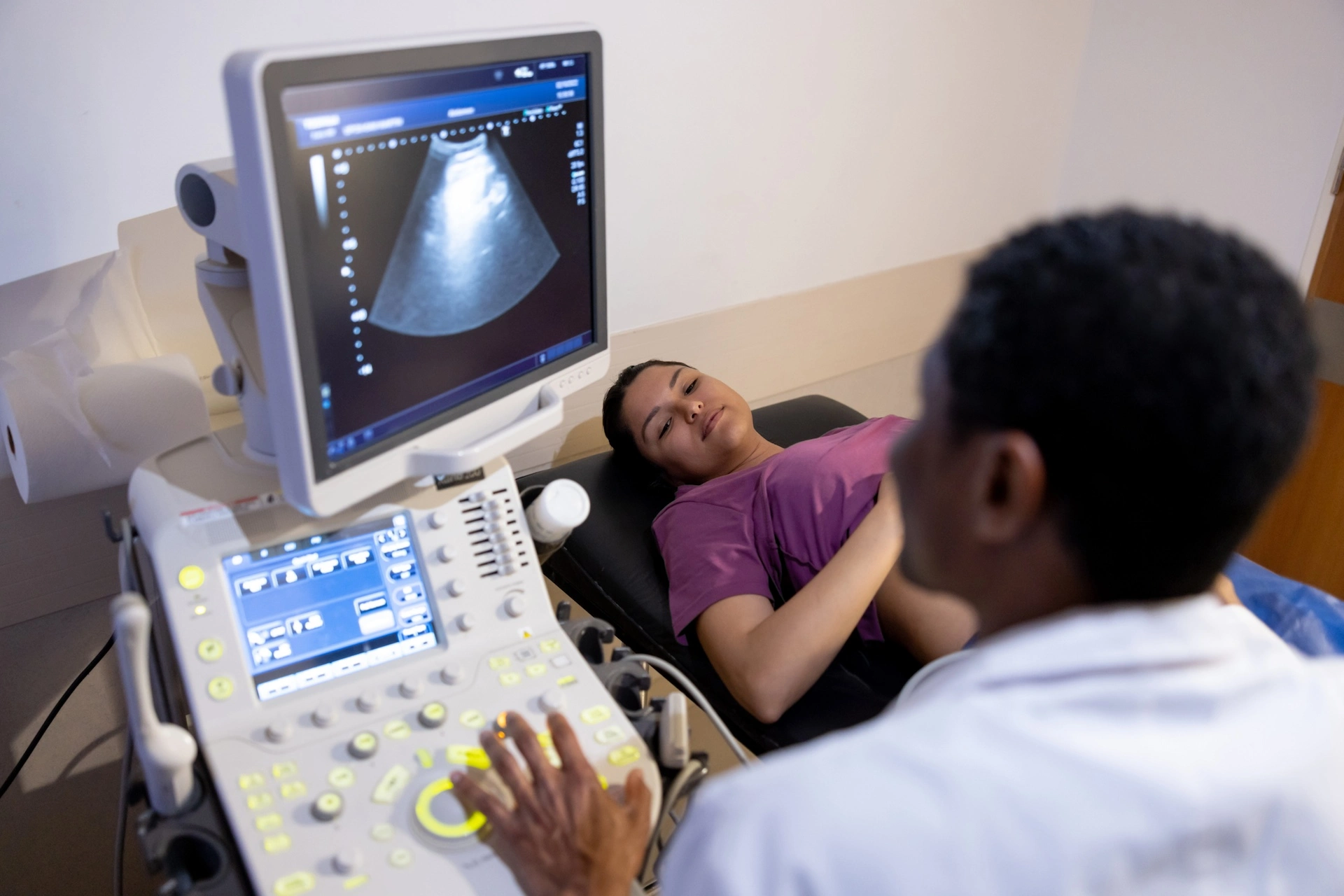
Betty Suh-Burgmann, MD, gynecologic oncologist at KP Walnut Creek and administrative chair of KP Northern California’s gyn-oncology subspecialty group, has been conducting research throughout her medical career and will now join the Physician Researcher Program to continue her work on optimizing the use of ultrasound and the detection of ovarian cancer. “The goal is to analyze our performance, implement a change and then analyze what happened from that change,” she says. “We see whether it worked out the way we thought, or maybe we’ve learned something new. It’s an iterative, ongoing learning process that doesn’t really end.”
Bridging from research to care delivery
During the first year, the physician researchers will meet with full-time investigators at the Division of Research several times a month for training, collaboration and consultation on their delivery science projects.
Douglas Corley, MD, PhD, MPH, director of the program, says physician interest was strong from the get-go. More than 60 physicians applied, and 16 candidates were invited to submit detailed proposals. One criteria for applicants was that they have some research experience.
“We’re not requiring people to be experts in research, but they need sufficient background for a rapid start,” Dr. Corley says. “We also wanted them to have institutional knowledge, established relationships within their specialty, and an understanding of the main clinical issues in Kaiser Permanente, so that they can work toward creating clinical change.”
Dr. Corley’s own TPMG career demonstrates how clinical practice integrated with research can work. He practices gastroenterology half-time at Kaiser Permanente’s San Francisco Medical Center, and conducts research the rest of the time at the Division of Research. His research program, funded primarily by competitive grants from the National Institutes of Health, focuses on improving screening for colorectal and other cancers, and the diagnosis and treatment of digestive diseases. He has authored or co-authored more than 150 peer-reviewed publications.
Likewise, Joseph Presti, MD, urologist at Kaiser Permanente in Oakland, has been conducting research throughout his medical career. Dr. Presti’s clinical and research work at Stanford University, the University of California, San Francisco and now Kaiser Permanente has focused on improving prostate cancer detection and screening techniques; he contributed significantly to the current 14-core biopsy scheme used to detect prostate cancer.
As part of the first class of physician researchers, Dr. Presti will focus on helping doctors and patients to assess prostate cancer risk and evaluate treatment options.
“With our large population of ethnically and racially diverse patients, we’ll be able to build a tool that takes all the critical clinical variables into consideration to assess one’s risk of prostate cancer,” Dr. Presti says. “Kaiser Permanente may be the only place in the world where this research can be done.”
***************************
ER doctors demonstrate the impacts of Delivery Science
When adults present to a hospital emergency department with a blood clot in their lungs, emergency room doctors usually arrange for hospital admission. But evidence from hospitals in Canada and Europe suggests that many of these patients can be treated just as effectively without hospitalization, saving them time and money and sparing them the risk of infections that comes with being hospitalized.
“Sorting out which patients with pulmonary embolism are suitable for home management can be tricky,” explains David Vinson, MD, co-chair of Kaiser Permanente’s CREST (Clinical Research on Emergency Services and Treatment) network of emergency medicine physicians. “The most reliable decision rule is complex, hard to remember and difficult to use.”
Repeatedly faced with this challenge, Dr. Vinson and members of the CREST network went to work.
“We developed a computerized version of the decision rule and integrated it with KP HealthConnect, with secure access to the patient’s electronic health record,” Dr. Vinson says. “This risk stratification tool, called RISTRA, can search the records and do all the fancy math in just a couple of seconds. With the click of a mouse, the treating physicians get the patient’s risk score and a suggestion about which site of care—home or hospital—is the safest for the patient.”
When the CREST researchers deployed RISTRA in some emergency rooms, but not in others, they found that safe home discharge rates increased by more than 50 percent. Because of those successful results, the RISTRA tool has recently been expanded to all 21 emergency departments in Kaiser Permanente Northern California.




This Post Has 0 Comments