Kaiser Permanente analysis finds non-adherent young women more at risk of pregnancy
Teens diagnosed with attention deficit hyperactivity disorder (ADHD) often don’t take their medication regularly, and new Kaiser Permanente research finds the problem gets worse when they hit adulthood.
The findings, published May 28 in the Journal of Adolescent Health, focused on ages 17 to 19 and shed new light on the specific types of patients who may be at risk of skipping treatment as they transition into a new stage of life, said lead author Kavitha Rao, MD, a child and adolescent psychiatrist with The Permanente Medical Group.
“The adolescent is striving for independence and making their own decisions and they may even question whether they have ADHD,” Rao said. “But ADHD affects executive functioning, organizational skills, time management, and being consistent with your daily living activities. All of these are impaired by ADHD. So of course that’s going to cause difficulties with adherence.”
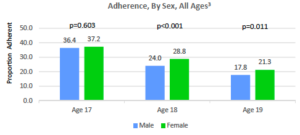
The study tracked 4,466 17-year-old ADHD patients for up to 2 years. At age 18, adherence to filling their prescriptions dropped from 36.7% to 25.6%, and at 19 it dropped further to 19%. Male patients, those with lower household incomes, and those with non-white race or ethnicity were less likely to maintain their prescriptions.
Health systems can also use the findings to support the transition from pediatric to adult care for teens, said senior author Cynthia Campbell, PhD, a research scientist with the Kaiser Permanente Northern California Division of Research. “That transition to adulthood is so key for many health conditions, not just ADHD,” Campbell said. “The continuity of care is really important. And Kaiser Permanente is well-positioned to focus on that.”
Rao and Campbell partnered with Diane M. Carpenter, MPH, Group Leader Data Consulting in the Division of Research’s Biostatistical Consulting Unit, on the analysis.
Adherence and specific outcomes
ADHD is a neurodevelopmental condition that involves developmentally inappropriate inattentiveness, impulsivity, and hyperactivity. ADHD in young adulthood is associated with high-risk behaviors and resulting health outcomes, such as accidents, sexually transmitted diseases, and substance use.
The analysis found female ADHD patients who kept taking their medication regularly (known as adherence) were less likely to have a pregnancy by age 19, and those who used any ADHD medication at all were less likely to have an injury or diagnosis of substance use at age 19. At all ages, white adolescents had the highest adherence rates, and the median household income was higher among those who filled their ADHD prescriptions more regularly.

Some of the most significant differences were seen in pregnancies; at age 19, 0.4% of ADHD patients who were adherent with their ADHD medication had a pregnancy, compared with 3.7% of those who were non-adherent. The authors said they couldn’t be sure if this was because the women discontinued their medication in anticipation of a pregnancy, but noted that most pregnancies at age 18 and 19 are unintended.
“It is plausible that untreated ADHD, with its associated executive functioning and self-regulation deficits, including poorer attention to safer sex practices, led to higher rates of both (sexually transmitted infections) and pregnancy in our female cohort,” the authors wrote.
Some teens may believe they will outgrow ADHD, but Rao said two-thirds of those diagnosed with ADHD in childhood will continue to have significant symptoms into adulthood.
In this study, “adherence” was defined as having filled a prescription covering at least 70% of the days prescribed. ADHD medication is generally prescribed daily; psychostimulants, which are most commonly prescribed, can also be taken as needed, as they work only on the day they are taken. Young people gaining independence judge for themselves when they need medication, Rao said.
 “The level of impairment from ADHD varies from day to day, depending on the environmental demands,” she said. “A patient may feel they don’t need it every day. I may argue as a clinician that they should take it every day, because their driving will be better, they may be less likely to have unprotected sex or abuse a substance. Having frank and collaborative discussion about how and when they take the medication is critical in engaging patients in treatment.”
“The level of impairment from ADHD varies from day to day, depending on the environmental demands,” she said. “A patient may feel they don’t need it every day. I may argue as a clinician that they should take it every day, because their driving will be better, they may be less likely to have unprotected sex or abuse a substance. Having frank and collaborative discussion about how and when they take the medication is critical in engaging patients in treatment.”
The analysis found lower risk of negative outcomes for patients who filled any amount of prescription versus those who filled none. “Even if they weren’t completely adherent, if they got prescribed any medicine at all, their outcomes were better than those who got none,” Rao said. “So somebody who took it 20% or 10% of the time had better outcomes than somebody who didn’t take it at all.”
For pediatricians and psychiatrists managing young patients with ADHD medications, the results suggest the importance of discussing medication and symptom management with their patients as they become more independent. “This involves a lot of detailed discussions and open communication,” Rao said.
The study was funded by the Kaiser Permanente Northern California Community Benefit Program.
# # #
About the Kaiser Permanente Division of Research
The Kaiser Permanente Division of Research conducts, publishes and disseminates epidemiologic and health services research to improve the health and medical care of Kaiser Permanente members and society at large. It seeks to understand the determinants of illness and well-being, and to improve the quality and cost-effectiveness of health care. Currently, DOR’s 600-plus staff is working on more than 450 epidemiological and health services research projects. For more information, visit divisionofresearch.kaiserpermanente.org or follow us @KPDOR.





This Post Has 0 Comments