Kaiser Permanente research also finds young people with autism use more health care services
Autism spectrum disorder is usually diagnosed in childhood, but the behavioral and communication challenges typically continue into adulthood. People with autism often have accompanying medical and psychiatric conditions, making for a complex history to pass on when transitioning from pediatric to adult care.

These challenges are explored in 2 research studies published recently in the journal Autism. The lead author was Jennifer Ames, PhD, a postdoctoral fellow with the Kaiser Permanente Division of Research; senior author was Lisa Croen, PhD, a research scientist who heads the division’s Autism Research Program.
“We wanted to know more about the health status of these young people, their experiences around the transition, and what physicians and other clinicians experience,” Croen said. So they surveyed 354 pediatric and 715 adult providers with Kaiser Permanente Northern California (KPNC). They also delved into KPNC electronic medical records to quantify health care usage by teens and young adults with autism (age 14 to 25), and compared them with groups of young people with and without chronic illnesses.
Croen and Ames answered questions about their latest research, which was funded by the WITH Foundation and Autism Speaks.
Q: What did you find out about health care usage of young people with autism?

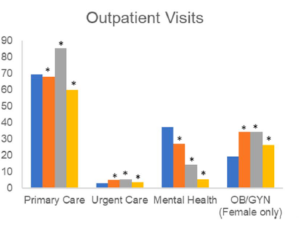
Ames: Youth with autism had high utilization of many service types we looked at, with service use generally similar to or somewhere in between youth with other chronic conditions such as attention deficit/hyperactivity disorder (ADHD) and diabetes. However, youth with autism had relatively high use of mental health services across the transition years, both in terms of visits to mental health providers and use of psychotropic medications. We know that individuals with autism have higher burdens of anxiety and depression. It’s important for them to have consistent mental health access.
We also found that individuals with autism had lower use of obstetrics and gynecology services than the control group or those with ADHD or diabetes. This suggests a disparity in using ob-gyn services — which we’ve also found among adults with autism — may start during the transition years. This is important to understand because female adolescents and adults with autism have unique experiences around their reproductive health and sexual health and really should be using ob-gyn as much as everyone else. We need to understand why they’re not going as often.
Q: What did you learn from surveying clinicians about their transition planning for children with autism?
Ames: The transition from pediatrics to adult care is particularly important for people with autism. We found the large majority of the departments and providers didn’t really have a consistent, coordinated approach to the transition. These include practices such as assessing the patient’s readiness to transition to adult care, making sure the patient is comfortable with their new provider, providing transition resources to families, and reviewing legal changes that come with being an adult, such as conservatorship.
Q: What should doctors be doing to bridge these patients to adult care?
Croen: A lot of these kids have co-occurring conditions and ongoing issues and you don’t want to have their healthcare fall through the cracks when they turn 18 and have to find a new doctor.
Ames: We found pediatricians raised medical transition questions with patients around age 17 or 18, while national guidelines support starting earlier, around ages 12 to 14. The families and providers need time to get themselves and the child ready for the transition.
Q: What has KPNC done to improve transitions of care for young people with autism?
Croen: Our survey was done in 2016, and in the meantime KPNC has certainly invested in improving the care transition. I was asked to work with a committee of pediatric subspecialists of The Permanente Medical Group called the Global Approach to Transition Experience and headed by pediatric pulmonologist Wan C. Tsai, MD. These specialists work with children with a variety of chronic conditions such as diabetes, cystic fibrosis, severe asthma, and other conditions for whom transition to adult care is particularly important.
The committee researched best practices for transition and built a protocol called Pedi-Adult Care Transition (PACT), a set of evidence-based tools that is being built into the electronic medical record to improve the transition from pediatric to adult providers.
Ames: PACT promotes use of transition-oriented healthcare visits starting at age 12 and creates lines of communication between pediatric and adult providers. It includes a medical summary, standardized assessments of transition readiness, and information about adult issues such as conservatorship easily accessible in an EHR tool called a smartset, which is a packaged set of orders and documentation.
Q: What other research do you plan on this topic?
Croen: We are actively pursuing funding to follow up on the findings about ob-gyn utilization, along with pregnancy in autistic women. Another interesting area we’d like to pursue is gender identity and sexual orientation in autism in both men and women.




This Post Has One Comment
This is a great collaboration. It would be helpful to teach clinicians how to communicate with young adults in the Spectrum (clear direct instructions, visual tools, etc.). As a mom with a kid in the Spectrum I want to say thank you for working on this important topic!