White patients much more likely than Asians to be diagnosed with the attention disorder, Kaiser Permanente research finds
The rate at which adults were diagnosed with attention deficit hyperactivity disorder (ADHD) doubled over ten years, increasing much faster than the diagnosis rate for children. That’s according to a new analysis of Kaiser Permanente patients in northern California.
The study also compared patients of various ethnic backgrounds and found younger white men were the most likely adults to be diagnosed with ADHD. The study was published Nov. 1 in JAMA Network Open.
The analysis examined records for nearly 5.3 million Kaiser Permanente members who received care in northern California between 2007 and 2016. It found the prevalence of ADHD in adults went from 0.43% to 0.96%, more than doubling, while diagnoses in children aged 5 to 11 increased from 2.96% to 3.74% (up 26%).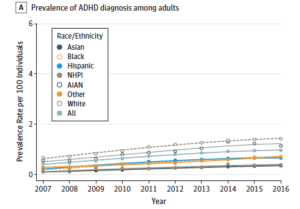
The research confirmed previous studies showing ADHD was found more often in whites than Asians, blacks, Hispanics, and Pacific Islanders. The analysis found yearly increases of ADHD prevalence among all ethnic groups studied, including a three-fold increase in Asians, from 0.11% to 0.35% of the study population.
The study was notable for the large number of patients and their racial and ethnic diversity, said lead author Winston Chung, MD, MS, a Kaiser Permanente psychiatrist in San Francisco, who collaborated with analysts with the Kaiser Permanente Division of Research. “There is a large population of people of Asian and other ethnicities here, so this is a unique opportunity to understand ADHD prevalence with a broad range of patient backgrounds,” he said.
The study did not determine the reason for the differences in prevalence, though Chung said there are a few possibilities: ADHD naturally occurs more often among certain populations, people from some cultures seek out care more, or providers are more likely to diagnose ADHD in certain groups.

Chung noted the potential for cultural influences on mental health disorders such as ADHD, with people in some cultures being less likely to see certain behaviors as a medical problem or to seek out help for them. “It’s always been just understood that different cultures and races might vary in meaningful ways in how they cope with stress or expressing emotions,” said Chung, who is associated with The Permanente Medical Group. “But this is something we don’t actually have definitive answers to,” he added, noting the need for more research to tease out the role of culture in mental illness diagnosis.
The study also found ADHD patients more likely to have eating disorders, depression, bipolar disorder, and anxiety. People diagnosed with ADHD were also more likely to have sexually transmitted diseases and frequent use of health care services. The authors said those findings are important to clinicians, who should consider the possibility a patient has additional “comorbidities” before prescribing stimulant medication.
The authors also cited the possibility of “diagnosis-seeking” among patients who may want ADHD stimulant drugs for “cognitive enhancement.”
The authors recommended continued work on screening tools that are unbiased, structured, and document ADHD symptoms over time to better understand and diagnose the disorder.
ADHD symptoms may include inattention, hyperactivity, and impulsivity starting in childhood. Chung said his adult patients with ADHD typically have trouble with completing tasks, are forgetful, distracted, or disorganized but may not have the restlessness associated with ADHD in children. The disorder is a top reason for adult outpatient psychiatric evaluations, he said.
Chung’s interest in the field known as cultural psychiatry prompted him to reach out to colleagues with deep knowledge of ADHD research at the Child Mind Institute in New York City, the National Institute of Mental Health, and New York University Langone Health to pursue the analysis, with support from the Kaiser Permanente Division of Research.
“Our findings, which provide important insights about recent trends in ADHD rates, confirm that there remains a large need to remove disparities in recognition of ADHD across ethnic groups,” said co-author Michael Peter Milham, MD, PhD, vice president of research at the Child Mind Institute. “As highlighted by our results regarding negative outcomes associated with ADHD, there are a range of costs to missing the diagnosis of ADHD that makes improved recognition critical.”
Funding for the research came from a Kaiser Permanente community benefit grant.
Co-authors also included F. Xavier Castellanos, MD, Brooke and Daniel Neidich Professor of Child and Adolescent psychiatry at NYU Langone Health in New York; Sheng-Fan Jiang, MS, from the Kaiser Permanente Northern California Division of Research; Diana Paksarian, PhD, and Kathleen R. Merikangas, PhD, of the National Institute of Mental Health; and Aki Nikolaidis, PhD, of the Child Mind Institute.





This Post Has 0 Comments