Kaiser Permanente study suggests medical management alone may reduce stroke risk in patients with severe asymptomatic carotid stenosis
The risk of having a future stroke caused by a severe blockage in an artery in the neck that is not currently causing any symptoms is so low that most patients with this condition — asymptomatic carotid stenosis — could potentially be treated with the newest medications and may not require surgery, new Kaiser Permanente research suggests.

“The question of how to best treat patients with narrowing of the carotid artery without symptoms has been a long-standing research priority,” said Robert Chang, MD, a physician researcher at the Kaiser Permanente Northern California Division of Research and a vascular surgeon at The Permanente Medical Group. “We decided to take a step back and to begin our study by asking how likely is it that these patients will actually have a stroke related to their severe stenosis. Our analyses showed that this risk is so low that it appears that, for most patients, surgery may not be necessary.”
The study, published May 24 in JAMA, is believed to be the largest and most current retrospective assessment of long-term stroke risk in this population. This type of study is rarely performed because it is difficult to have access to sufficient current information about patients with this condition.
Carotid stenosis occurs when plaque — fatty cholesterol deposits — builds up in one or both of the large arteries on either side of the neck that carry blood to the brain, face, and head. This narrowing in the artery is typically diagnosed after a patient has experienced symptoms of a stroke, but it can also be found during a routine physical examination. When the condition is found incidentally, and not after a stroke or other neurologic event, the diagnosis is asymptomatic carotid stenosis.
 Randomized clinical trials conducted prior to 2010 concluded surgery to remove the blockage was the best option for reducing stroke risk in patients with severe stenosis. For many years these studies have guided clinical care. But as medical treatments for reducing stroke risk have improved, physicians have begun to wonder whether surgery should remain the preferred treatment for asymptomatic patients.
Randomized clinical trials conducted prior to 2010 concluded surgery to remove the blockage was the best option for reducing stroke risk in patients with severe stenosis. For many years these studies have guided clinical care. But as medical treatments for reducing stroke risk have improved, physicians have begun to wonder whether surgery should remain the preferred treatment for asymptomatic patients.
A population-based research approach
To answer that question, Chang and his colleagues identified 3,737 Kaiser Permanente members in Northern California who had been diagnosed between 2008 and 2012 with severe (70% to 99% blockage) asymptomatic carotid stenosis. None of these patients had previously had surgery.
The question of how to best treat patients with narrowing of the carotid artery without symptoms has been a long-standing research priority.
— Robert Chang, MD
The research team first looked to see how the stenosis had been treated. Reviewing the patients’ medical records showed 1,423 patients had surgery to treat the stenosis and 2,314 had not. The team also tracked which patients were taking a statin (a drug used to help lower cholesterol in the blood) or medication to reduce high blood pressure. Then they looked to see which patients had a carotid-related stroke on the same side as the severe carotid stenosis, following the patients through 2019.
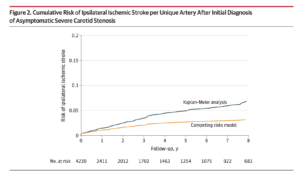
Overall, 133 strokes were diagnosed in 129 patients during the follow-up period. Statistical analyses showed the patients who did not have surgery had a 4.7% cumulative risk of having a stroke within 5 years of their carotid stenosis diagnosis. The risk was higher in patients who were older and had a larger blockage; it was lower in patients who were on a statin. The study also reported favorable trends in blood pressure and cholesterol control that were likely related to Kaiser Permanente’s emphasis on prevention.

The study’s senior author, Mai N. Nguyen-Huynh, MD, MAS, a research scientist at the Division of Research and regional medical director for primary stroke with The Permanente Medical Group (TPMG), said the findings did not surprise her. “We suspected that we may find a low risk of stroke in these patients because there are now better stroke-prevention treatments, including medications to control blood pressure, prevent blood clots, and reduce cholesterol, than we had when the original randomized trials were done more than a decade ago that led to the conclusion surgery was the best treatment,” she said.
Chang said that Kaiser Permanente’s integrated approach to medical care along with its large, representative membership made it possible for their team to conduct a population-based study to estimate the risk for a carotid-related stroke. He and Nguyen-Huynh also currently head up a team at the Division of Research affiliated with a national randomized clinical trial comparing surgery or stenting to medical management in patients with asymptomatic carotid stenosis.
One limitation of their new study, said Chang, is that it included only members of Kaiser Permanente Northern California. “We can’t say that our findings would be the same for a population that, for example, doesn’t have regular access to medical care or that lives in geographic regions with high smoking rates, which increases stroke risk,” he said.
Even so, Nguyen-Huynh said, “I think our study will make many patients and their doctors think twice about surgery if they can instead be on an effective, aggressive medical management program to lower their stroke risk from asymptomatic carotid disease.”
Chang said that Kaiser Permanente’s integrated approach to medical care along with its large, representative membership made it possible for their team to conduct a population-based study to estimate the risk for carotid-related stroke. He and Nguyen-Huynh also currently lead a team at the Division of Research affiliated with a national randomized trial, called CREST2, that is enrolling patients in a study comparing surgery or stenting to medical management in patients with asymptomatic carotid stenosis. “This head-to-head comparison of carotid surgery versus medical management in a clinical trial is what we need to help us determine the appropriate approach,” said Nguyen-Huynh.
The study was funded by The Permanente Medical Group’s Delivery Science and Applied Research Program.
Co-authors include Andrew L Avins, MD, and Lue-Yen Tucker, BA, of the Division of Research; Alexander C Flint, MD, PhD, of the Division of Research and The Permanente Medical Group; Kara A Rothenberg, MD, of the University of California San Francisco – East Bay; Elizabeth Lancaster, MD, MAS, of the University of California, San Francisco; Rishad M Faruqi, MD, and Hui C Kuang, NP, of The Permanente Medical Group.
# # #
About the Kaiser Permanente Division of Research
The Kaiser Permanente Division of Research conducts, publishes and disseminates epidemiologic and health services research to improve the health and medical care of Kaiser Permanente members and society at large. It seeks to understand the determinants of illness and well-being, and to improve the quality and cost-effectiveness of health care. Currently, DOR’s 600-plus staff is working on more than 450 epidemiological and health services research projects. For more information, visit divisionofresearch.kaiserpermanente.org or follow us @KPDOR.





This Post Has 0 Comments