Kaiser Permanente Center for Thoracic Aortic Disease study confirms low long-term risk for most aneurysms
A diagnosis of a thoracic aortic aneurysm — a bulge in the part of the main artery that runs through the chest — can be frightening. Learning that a complicated surgery may be necessary to prevent the aorta from tearing and leaking blood into the body, only adds to the shock. But a large, new Kaiser Permanente study provides high-quality evidence that most of the 33,000 patients diagnosed each year in the U.S. with a thoracic aortic aneurysm are not likely to experience a tear or rupture — an aortic dissection — and may not need open-heart surgery.

“We built the largest-ever cohort of patients with thoracic aortic aneurysm to study their natural history,” said lead author Matthew D. Solomon, MD, PhD, a physician researcher at the Kaiser Permanente Division of Research and a cardiologist at The Permanente Medical Group. “This research was critical because of the paucity of evidence to guide clinicians and the ongoing debate in the field as to how large an aneurysm should be before recommending a patient undergo a very high-risk surgery.”
The study, published October 5 in JAMA Cardiology, is the largest to date to support the current consensus guidelines that recommend surgery for most patients with a thoracic aneurysm that is 5.5 centimeters or larger. These guidelines are specific to patients who do not have certain genetic conditions that increase their risk of experiencing an aortic aneurysm or dissection.
The study included 6,372 patients in Kaiser Permanente Northern California (KPNC) who were identified as having a thoracic aortic aneurysm between 2000 and 2016. Of these, 6,092 (96%) were diagnosed with an aneurysm that was initially less than 5.5 centimeters, and 280 (4%) were initially diagnosed with an aneurysm 5.5 centimeters or larger. All the patients were enrolled in a computerized population management system to ensure patients received appropriate, ongoing imaging to assess the size and growth of their aneurysm. None had a genetic syndrome known to increase risk for an aortic aneurysm or dissection.
Our study will help physicians and patients make the most informed decision when contemplating such a significant procedure.
— Matthew D. Solomon, MD, PhD
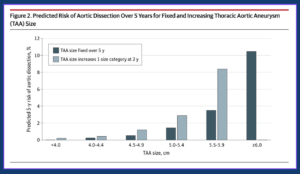
For patients with an aneurysm less than 5.0 centimeters, the 5-year risk of experiencing an aortic dissection was less than 1%, and for those 5.0 to 5.4 centimeters, it was 1.5%. But for patients with an aneurysm 5.5 centimeters or larger, the story changed: The 5-year predicted risk of dissection for an aneurysm 5.5 to 5.9 centimeters was 3.6%, and for those with an aneurysm 6 centimeters or larger, the 5-year risk of experiencing a dissection jumped to more than 10%.
“Our study shows that regular monitoring, coupled with aggressive blood pressure control and lifestyle changes, is a safe strategy for most patients until the aneurysm reaches the 5.5 centimeter mark, when surgery becomes necessary,” said Solomon, who is the founder and director of the KPNC Center for Thoracic Aortic Disease. “The fact that we found a clear inflection point in risk at 6.0 centimeters supports the current guidelines and will help inform the debate of when to do surgery.”
A complex surgery
The aorta, which is about the diameter of a garden hose, is the largest blood vessel in the body. It carries blood from the heart to all the vital organs. A thoracic aortic aneurysm typically causes no symptoms and is usually discovered incidentally, on a scan for another health problem.
 Skilled cardiac surgeons can perform surgery to repair the aneurysm to prevent a dissection. But it is a complex procedure that can require stopping the heart and putting patients on a heart-lung bypass machine to replace the heart’s pumping function. The surgery can put patients at risk for a heart attack, stroke, pneumonia, and loss of kidney function; requires a hospital stay of up to 10 days; and has a recovery time of 2 to 3 months.
Skilled cardiac surgeons can perform surgery to repair the aneurysm to prevent a dissection. But it is a complex procedure that can require stopping the heart and putting patients on a heart-lung bypass machine to replace the heart’s pumping function. The surgery can put patients at risk for a heart attack, stroke, pneumonia, and loss of kidney function; requires a hospital stay of up to 10 days; and has a recovery time of 2 to 3 months.
“We have amazing cardiac surgeons and an outstanding aortic surgical program, but this can be one of the most difficult surgeries they do,” said Solomon. “Patients absolutely need this surgery when surgical risk is less than the risk of dissection. Our study will help physicians and patients make the most informed decision when contemplating such a significant procedure.”

Started in 2017, the Kaiser Permanente Center for Thoracic Aortic Disease includes a multispecialty team of cardiologists, cardiac surgeons, vascular surgeons, geneticists, nurses, and imaging analysts. The team cares for nearly 15,000 KPNC patients through its groundbreaking population management program and has presented its work and shared best practices nationally and internationally.
“This type of study in a very large diverse population where patient characteristics, care received, and outcomes experienced are systematically captured across practice settings is only possible within a fully integrated health care delivery organization like Kaiser Permanente,” said senior author Alan S. Go, MD, a senior research scientist at the Division of Research. “The ability to do these long-term follow-up studies among representative patients is critical to informing accurate risk prediction and optimizing management decisions for thoracic aortic aneurysm.”
The study was supported by Kaiser Permanente Northern California Community Health and The Permanente Medical Group’s Delivery Science and Applied Research Program.
Co-authors include Thomas Leong, MPH, Sue Hee Sung, MPH, Catherine Lee, PhD, of the Division of Research; J. Geoff Allen, MD, Joseph Huh, MD, Paul LaPunzina, MD, Hon Lee, MD, Duncan Mason, MD, Vicken Meliklan, MD, Daniel Pellegrini, MD, David Scoville, MD, PhD, Ahmad Y. Sheikh, MD, Dorinna Mendoza, MD, Sahar Naderi, MD, Ann Sheridan, MD, Xinge Hu, MD, PhD, Wendy Cirimele, BSN, MPA, Anne Gisslow, RN, MSN, Sandy Leung, RN, Kristine Padilla, RN, Michael Bloom, MA, Josh Chung, MD, Paniz Vafaei, MD, and Robert Chang, MD, of The Permanente Medical Group; Adrienne Topic, MD, of Wellspan Health; and D. Craig Miller, MD, and David H. Liang, MD, PhD, of Stanford University for the Kaiser Permanente Northern California Center for Thoracic Aortic Disease.
# # #
About the Kaiser Permanente Division of Research
The Kaiser Permanente Division of Research conducts, publishes and disseminates epidemiologic and health services research to improve the health and medical care of Kaiser Permanente members and society at large. It seeks to understand the determinants of illness and well-being, and to improve the quality and cost-effectiveness of health care. Currently, DOR’s 600-plus staff is working on more than 450 epidemiological and health services research projects. For more information, visit divisionofresearch.kaiserpermanente.org or follow us @KPDOR.





This Post Has 0 Comments